On July 1 voluntary assisted dying became legal in WA, marking the end of a prolonged campaign by dying with dignity advocates and members of the public. At the end of the month, on July 29, history was made when it was announced the first West Australian had made use of the assisted dying service.
But months after all the celebration, how is the implementation of VAD laws in our health system tracking along?
According to the experts, there is a shortage of medical professionals who have registered and completed the training to work as VAD practitioners across the state, leaving the few who have with a burdensome responsibility. Access to VAD remains limited, particularly in regional areas.
Dying with Dignity president and lawyer Stephen Walker has long advocated for these rights, and as we sit in his Mosman Park home, he describes his mixed emotions surrounding the state’s VAD situation.

According to Mr Walker, the WA VAD system is having a “bit of a slow start” with the particular concern being the lack of medical professionals who have completed the required training to be a coordinating or consulting practitioner of VAD.
The numbers published in Hansard from September 16, 2021 showed just 38 doctors and no nurses were registered and trained to be involved with VAD across the state.
“We see improvements that could be made and we want to work towards those improvements, particularly bearing in mind that in only two years or so, there will be a review of the Act.”
Stephen Walker, Dying with Dignity
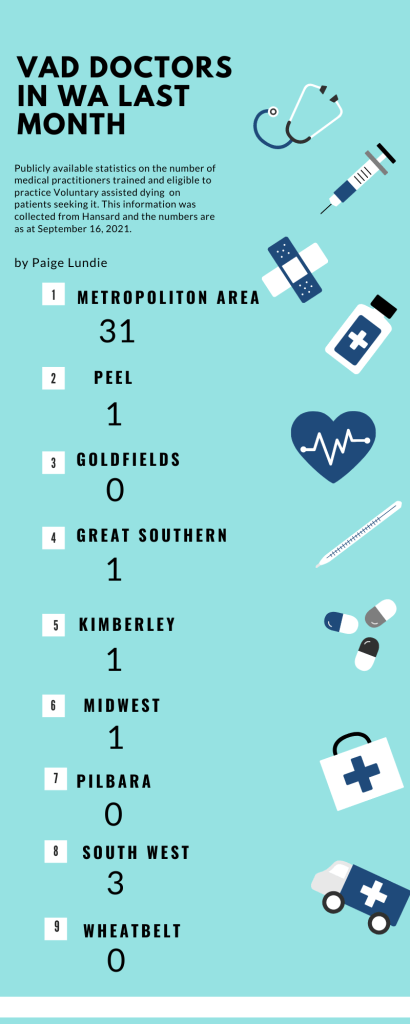
Last month, the figures showed there were no local doctors who could help a patient with voluntary assisted dying in the Goldfields, Pilbara and the Wheatbelt.
In the lead up to July 1, chair of WA voluntary assisted dying implementation team, Dr Scott Blackwell told the ABC that VAD was “unlikely to be widely used” once it became legal.
As at September 16, 2021 there had been 172 first requests submitted for voluntary assisted dying and 33 people have died via VAD administration in West Australia.
While in proportion to the population the number of requests is low, Doctors for Assisted Dying Choice WA convener Dr Richard Lugg says the current number of doctors registered and trained as consulting and/or coordinating practitioners is insufficient to meet the demand.
Lugg says the majority of the 33 VAD administrations that have occurred in WA so far have been done by just a small pool of doctors.
According to Lugg, the nature of the work can be emotionally draining for those doctors.
“Those doctors who are doing, picking up the bulk of the work, they are to be quite honest, they’re struggling.”
Dr Richard Lugg, Doctors for Assisted Dying Choice.

So how are patients seeking VAD in regional areas accessing the service when there are no local VAD practitioners?
A State wide care navigator service (SWCNS) is a nurse-led program put in place by the WA Health Department to provide West Australians with support, information, advice and assistance to connect with VAD trained doctors and nurses.
Care navigators involved in SWCNS also run the Regional Access Support Scheme, a system established to provide financial aid for access to assisted dying to those living outside the metropolitan area.
The scheme is designed to aid patients in regional areas to travel to a metropolitan area or for a practitioner to travel to them for consultation and administration of VAD if they seek it.
According to the Department of Health, the Regional Access Support Scheme has been used multiple times since July 1.
One doctor who has had experience with this service is Angela Cooney. Cooney has worked as a general practitioner in Perth for nearly 30 years. She is one of the few doctors in WA who is registered and trained to relieve people from pain and suffering through voluntary assisted dying.
As we’re sitting in the garden area of a quaint Nedlands cafe, Cooney explains why this work is so important to her.
“I guess it has just fitted in very well with the other areas that I work in which is all about giving people choices in their lives,” she says.
Due to there being no trained VAD practitioners in the Goldfields region, Cooney has been flown out to Esperance multiple times in recent weeks to help residents seeking VAD.
Cooney is tired. It’s been a rough week for her. As she sips her well-needed coffee she begins to describe a harrowing situation with one regional patient whose VAD request was delayed, leaving him desperate for relief that was hundreds of kilometres away.
Due to their being no VAD practitioners in the Goldfields region, Cooney put up her hand to travel to a patient and give him the required assessment for VAD eligibility before she could return to eventually assist with administration. But according to Cooney, the man’s initial request had been delayed leaving him desperate for immediate relief.
“He was so ill. On my way back to the airport I contacted the care navigators and the pharmacist and said ‘I have to get back to this man as soon as possible or else he’s going to be dead’.”
Cooney says due to it being school holidays there were some obstacles involved with getting a flight but eventually she got on a plane from Perth to the Goldfields, but it was an anxious journey as she was unsure whether or not the patient would still be alive by the time she landed.
“He could easily have died within a couple of hours anyway so in that way I was too late because he had so much more misery than he could have.”
According to Cooney the situation likely would have turned out differently if there was a local doctor that could have helped instead.
“He would probably have ended his life two or three weeks earlier and not have had to lose the 30 kilos in weight that turned him into a living skeleton with misery. It was so sad to see somebody in that state. So it was the delay that was the horrible thing for him. He had been asking and asking for months.”
Dr Angela Cooney
An information sheet provided by the WA Health Department outlines the requirements involved for a medical practitioner to administer voluntary assisted dying training. Just some of the criteria listed includes that the qualified medical practitioner must have at least five years experience as a specialist and must have completed at least 12 months work in a supervised position in WA before they can register.
Cooney says the strict eligibility criteria for medical practitioners to participate in VAD is proving to be a direct obstacle for one regional doctor and could be holding back others interested.
“I do know that there is a doctor in Esperance who would love to be involved, however, his recent arrival from overseas does not qualify him to be able to do the training yet, so I’m sure he will, but it may be two years down the track,” she says.
One requirement which is exclusive to WA, is that each practitioner must provide two professional referees to the End of life Care Program for verification and approval.
Richard Lugg has concerns the two referee requirement is discouraging doctors from signing up.
According to Lugg, there are many doctors who would like to offer continuity of care to their established patients by getting trained for VAD, however they don’t want to broadcast it outside of their patient pool and get flooded by others seeking the service. Due to many medical practitioners wanting to keep it quiet the two referee requirement is turning some away.
“So those people want to keep it sort of fairly quiet and talking to fellow professional colleagues is something that some of them really don’t want to do. We know this, we’ve heard people say this,” he says.
“And then there are other problems. The training that’s required, is quite intensive. The estimate is it will take a doctor at least six hours sitting at a computer screen to get through all the modules involved and I know of doctors that have taken considerably longer than that, breaking it up because how many doctors have six hours straight to sit down and look at a computer?”
Down in the cozy, regional, south west town that is Augusta, retired doctor, Wayne Pennington who spent most of his career as a rural medical practitioner in a remote Victorian town, says it is a blessing that this service is now legally available but he is puzzled by the amount of training required.
“It’s an absolute blessing. It’s something that should have happened when I was young, you know, because it was just such an obvious thing.”
Dr Wayne Pennington, retired doctor
“What training do you need? You’ve just got to make sure you keep someone really comfortable and you just do the right thing as far as I’m concerned.”
A spokesperson for the Department of Health WA says the department has not received any feedback from medical practitioners that the two-referee requirement has been a disincentive for registering and completing the training for VAD.
“The referee check is an opportunity to confirm the clinical skills of the practitioner and highlight any issues that may impact the practitioner’s ability to support patients through an emotionally challenging process,” the spokesperson says.
“The department is currently working with key stakeholders on several strategies to encourage and support medical practitioners to complete the approved training and assist patients seeking to access voluntary assisted dying.”
According to the Department of Health WA, this month there are an additional three medical practitioners registered and trained across the state including one in the Pilbara.
Health Consumers Council executive director, Pip Brennan says it’s important to remember that it is only October and the reluctance we are seeing among doctors may be to do with fear around it being unfamiliar territory.

“There would be some people who might over time feel more comfortable as they see it actually happening, because, you know, you’ve got to remember, it’s so new, and there could be all sorts of unintended consequences,” she says.
Brennan says it is also important to approach this area with caution and the restrictions and safeguards are important aspects to the legislation.
According to Brennan, the concept of ableism has some worried that coercion might begin to creep in toward those with disabilities.
“Look, it’s really important that this is there but I think we also have to remember that there is this need to be careful. We need to understand the perspective of that whole frame around healthcare where ableism is actually a thing. It’s definitely a thing,” she says.
Sir Charles Gardner Hospital Emergency physician Dr Gareth Wahl has been involved with 13 patients seeking out VAD in WA and has so far assisted seven people to die voluntarily in the state.
Wahl says the key to better accessibility to voluntary assisted dying is more education in the health care system. From what he’s seen so far, there are a lot of patients making requests for VAD and not being heard.
“A lot of patients are saying, ‘I want you to help me die’ and are not necessarily being heard when they’re saying that by doctors and nurses, etc. It’s taking a little while for them to get to getting in touch with someone who’s able to help them.”
Dr Gareth Wahl, Sir Charles Gardener Hospital
The Voluntary Assisted Dying Act 2019 does not prevent entire institutions conscientiously objecting to voluntary assisted dying. This means institutions which are ethically opposed to voluntary assisted dying can choose to not allow any staff or person to be involved in the administration of VAD on site.
“So you can imagine that anything that is Catholic based is particularly an issue and I wouldn’t name institutions, but I’m sure you can imagine. That is an issue because a lot of palliative care is run by faith based institutions. Patients who are accessing this are often involved with— all of my patients have had some involvement with palliative care and there’s a real limited number of palliative care beds that are not in faith based institutions, which makes it difficult for patients to access VAD,” Wahl says.
Wahl says while there is an emotional toll involved in this work he also experiences emotional reward.
“I think this is a really important thing to be able to give patients at the end of their life. I think, everybody is busy, but I think there is an obligation on people to be involved,” he says.
One man who is working to reinvent the discussion around death and dying is ‘Dying out Loud’ founder, Dave Warnock. Warnock lives in Charlotte, North Carolina in the United States and has been diagnosed with an incurable terminal illness, ALS (motor neuron disease).
The right to die with dignity is an issue that hits close to home for Warnock, but he says the dying with dignity laws in the few states where it is legal in the US are so restrictive that he isn’t interested in them, leading himself and others seeking a death with dignity toward the Final Exit Network. The Final Exit Network is a not for profit advocacy group that works to help those who need it, access a death with dignity regardless of the state or country they reside in.
According to Warnock, just some of the criteria required for someone to access a death with dignity in the few US states where VAD is legal, include that a doctor must confirm the patient is within six months of death. Similar restrictions apply in WA with patients seeking VAD only eligible if they are terminally ill with just 6 months left to live and 12 months for those with a neurodegenerative illness.
Warnock says it is his view that these obstructions are primarily in place because of religious opposition and restrictive VAD laws aren’t helping anyone.
“I should decide when the quality of my life has reached a level that’s just not satisfactory.”
Dave Warnock, ‘Dying out Loud’.
Despite the controversial nature of voluntary assisted dying, experts have found no stigma among the Australian population in relation to VAD.
Curtin School of Population Health associate professor Dr Lauren Breen says grief is subjective and complex, and while it’s possible families of individuals using the new voluntary assisted dying laws in WA could have more opportunity for preparedness, there’s no way to know for sure how each individual will grieve the death of a loved one.
“We don’t know very much yet about the impact on people in Western Australia or in other parts of Australia, so what we can do is look to where it’s been legal for longer in other places and the impact on people grieving there, and one of the main things is around — people often feel like they might have to engage in secrecy management around the cause of death,” Breen says.
Lifeline is available 24-hours on 13 11 14.

